Culturally adapted validated translation of the NIHSS
The translated NIHSS form and guide remain true to the English version and are harmonised with the non-validated Norwegian version.
Background: The National Institutes of Health Stroke Scale (NIHSS) is an internationally recognised screening tool used by healthcare professionals to record neurological outcomes of patients with a suspected stroke. The scale has been used by nurses and doctors in stroke units in Norway since the 1990s. The Norwegian version of the NIHSS that is currently in use has not been validated.
Objective: To give an account of the culturally adapted validated translation of the NIHSS.
Method: In collaboration with the University of South-Eastern Norway and a qualified translator, a project group consisting of nurses and doctors from stroke units in Vestre Viken Hospital Trust produced a culturally adapted validated translation of the NIHSS. The translation process followed the steps in the modified translation method of the Regional Competence Centre for Pain (ReKS). We conducted a pilot test with several stroke units.
Results: The terminology in the validated NIHSS largely matched that of the non-validated version. The descriptor ‘IT’ in the validated version corresponds to the original version. Illustrations and text sheets from the original NIHSS were included in the validated version with a few adjustments. Total score and time spent administering the scale were comparable to the non-validated version.
Conclusion: Validation of the NIHSS was required to ensure cultural adaptation and that the language was consistent with the original English version. Involving stroke units, conducting a pilot test and putting together a project team of experienced doctors and nurses were important factors in the validation process. The result is a Norwegian validated version of the NIHSS and guide that is true to the original English version and at the same time harmonised with the non-validated existing Norwegian version.
The National Institutes of Health Stroke Scale (NIHSS) is an international stroke scale used by healthcare professionals to record neurological outcomes in suspected strokes and to monitor symptom development (1-5). The NIHSS was developed in 1989 and subsequently revised in 2003 (2).
Nurses and doctors in stroke units in Norway have been using the tool since the 1990s. The eleven different functions that are scored are level of consciousness, LOC questions, LOC commands, best gaze, visual, facial palsy, motor arm and leg, limb ataxia, sensory, best language, dysarthria and neglect.
An NIHSS score provides information on the severity of the stroke and goes from score 0 (no outcome), score 1–4 (minor stroke), score 5–15 (moderate stroke), score 16–20 (moderate to severe stroke) to score 21–42 (severe stroke) (6).
The original English NIHSS form and guide includes illustrations and text sheets. The guide is a detailed description of how the NIHSS should be administered in practice, and how to score (2, 7). Several countries have developed culturally adapted validated translations of the NIHSS in their own language, including illustrations (8, 9).
Background for the translation
The stroke units in Vestre Viken Hospital Trust have had a common clinical pathway for the treatment of stroke patients since 2002. A long-standing collaboration is in place between the stroke units and the University of South-Eastern Norway (USN) to provide clinical practice placements for nursing students and for students taking postgraduate studies in strokes, where training in the use of NIHSS is an important part.
In connection with this collaboration, discrepancies emerged in the scoring of patients, which led to questions being asked about the standard of the training in the NIHSS. A project group was established, consisting of a doctor, four nurses from the stroke units in Vestre Viken Hospital Trust and a lecturer from USN.
The aim of the project was to develop an e-learning course in Norwegian in order to standardise the training. As part of this work, we found that the Norwegian version of the NIHSS, which has been used in clinical practice for a number of years (1), has not been validated according to the standard method (10).
There is no consensus on how a screening tool should be adapted to another culture, but there is agreement that a mere direct translation is insufficient (11, 12). Because an e-learning course was to be developed, the project group decided to first produce a validated translation of the NIHSS.
Objective
The objective of the article was to give an account of the culturally adapted validated translation of the NIHSS.
Method
The validated translation process followed the steps in a modified translation method for questionnaires, which was developed at the Regional Competence Centre for Pain (ReKS), Department of Pain Management, Oslo University Hospital (13). The method is supported by the World Health Organization (WHO), which has also developed a method for producing validated translations (10).
The method starts with a preparation phase, consisting of a forward translation and a back translation. Harmonisation and a pilot test are then performed as part of a cognitive debriefing process. The last step is the finalisation phase. This translation method was chosen as it is in line with the recommendations for validated translation work (10).
ReKS defines the different roles for the professionals involved (13), such as chief consultant, forward translator and project manager. In this project, five professionals formed an expert panel that undertook all of the roles.
The use of an expert panel is recommended for translation work (10). The expert panel consisted of three stroke nurses: two with a postgraduate qualification in neurology and one with a master’s degree in nursing. The panel also consisted of a senior consultant neurologist and a senior lecturer in nursing with experience in the treatment of strokes. In addition to the expert panel, four forward translators and a qualified translator undertook defined tasks.
The preparation phase
In the preparation phase, we contacted the licensee, the National Institute of Neurological Disorders and Stroke (NINDS), to clarify any conditions for the translation from English to Norwegian. The response was that the original version had to be referenced in the final product.
The expert panel reviewed the original version of the NIHSS. The goal was to identify words and terms, both in the form and the guide, that would be challenging to translate.
Forward translation
According to ReKS, the criteria for forward translators were that their first language was Norwegian, they can write and speak English, and that they preferably have experience with validated translation work (13). There were four forward translators involved in the project: a nurse from a stroke unit, a doctor from a stroke unit, a university lecturer with knowledge of strokes and validated translation work, and a nurse with research experience and experience with validated translation work.
Three of the four had Norwegian as their first language, and one was a native Danish speaker with 30 years of experience with the Norwegian language. All four could write and speak English. The forward translators noted challenges and tried to make the text understandable and adaptable to Norwegian. The forward translators translated the NIHSS and the guide from English to Norwegian without any form of collaboration.
The purpose of the forward translation was to make the text understandable and adaptable to the Norwegian language, culture and discipline as opposed to a literal translation. In line with the translation method, the expert panel discussed with the forward translators whether the illustrations and text sheets used in the original version were recognisable themes in Norwegian culture.
The expert panel reviewed the forward translations without knowing which translator had carried out which translation, and together developed the first Norwegian translation.
Back translation
A qualified translator was recruited. The criteria for the qualified translator were English as a first language, fluent written and spoken Norwegian, and that they had medical knowledge (10, 13).
The qualified translator should have no knowledge of the text to be translated, and must focus on concepts within a cultural context as opposed to a linguistic framework (10). The qualified translator who back translated the NIHSS form, the guide and the text sheets met the requirements.
Harmonisation
The expert panel reviewed and discussed the back translation from Norwegian to English. According to ReKS, the original author should participate in this part of the process. The original author did not participate in this project because the text was developed by several authors in collaboration.
The NIHSS was developed by a national institute of neurological conditions and strokes. The main purpose of the work was to compare terms and concepts between the original and the translated version of the NIHSS.
The expert panel had a dialogue with the qualified translator about some concepts that needed to be adjusted in line with the original version of the NIHSS. It was also crucial to ensure that the Norwegian version was culturally and linguistically adapted to Norwegian conditions.
Following the collaboration with the qualified translator, the expert panel prepared a second Norwegian version of the NIHSS. The harmonisation process involved comparing the validated and the non-validated versions of the NIHSS in Norwegian.
The comparison included a discussion on linguistic differences, both in the NIHSS form and the guide. It was also important to ensure that the validated guide was precise and applicable in practice. Following the comparison, the expert panel produced a third Norwegian version of the NIHSS.
Cognitive debriefing
ReKS describes cognitive debriefing as a test of the finished product (13). The expert panel sent out a preliminary version to nine stroke units. Six stroke units participated in the pilot test, which included 29 stroke patients. WHO points out that it is crucial that the pilot test respondents are representative of the population on which the screening tool will be administered in practice (10).
Pilot testing is useful for ensuring the content validity, face validity and reliability of the validated version of the NIHSS and attachments (14). Two healthcare professionals (herein referred to as test subjects) - either two nurses or one nurse and one doctor from each of the six stroke units - tested the same patient using the non-validated version.
Both tested the same patient at the same time to ensure they had the same understanding of the tool, and thus consistent approaches to scoring. One test subject then used the validated version and the other used the non-validated version on the same patient at the same time, and subsequently compared scores.
The test subjects provided written feedback on whether there were any words and terms in the NIHSS and guide that were difficult to understand, and whether the text sheets and illustrations could be used.
Completion
The expert panel reviewed all submitted responses and made changes to words and sentences that were deemed necessary to understand the NIHSS form, the guide, the text sheets and the illustrations. The panel then prepared the fourth version of the NIHSS.
The final step in the validation process was to finalise the NIHSS form and guide, text sheets and illustrations by proofreading and adjusting the text.
Results
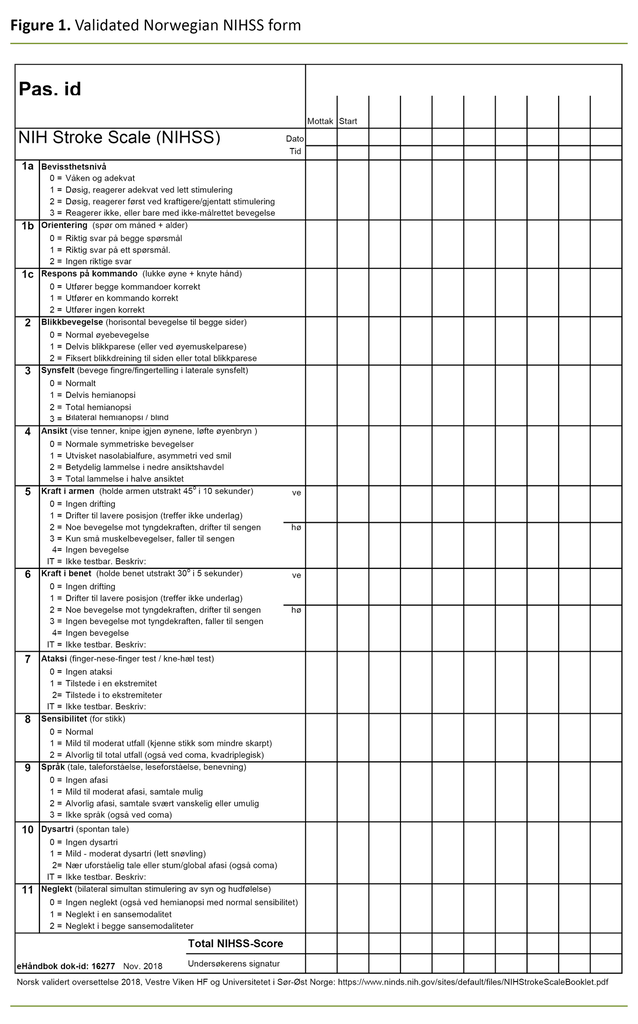
The presentation of the results of the translation process and subsequent pilot testing follows the structure and order of the NIHSS form. Choices that we made during the translation process are highlighted in the presentation. The validated translation of all points in the NIHSS form is presented. Figure 1 shows the result of the validated Norwegian NIHSS form. (Appendix 1 shows the original English NIHSS form.)
Concepts that were recognisable in practice
We identified terms in both the NIHSS form and the guide that were interpreted in different ways. One forward translator deliberately used as general language as possible in the translation, in order to make it easy for the clinician to understand the meaning. Terms in the English NIHSS form that were challenging to translate into Norwegian are shown in Table 1.
All forward translators found it difficult to translate the term ‘alert’, which is used in the original version to describe the level of consciousness. It was not only the level of alertness that was difficult to define, but also what type of response could be expected for the different levels of alertness.
The four forward translators each suggested a different Norwegian translation (våken og klar, målrettet respons, våken og oppmerksom, and våken og adekvat). The expert panel discussed the Norwegian term adekvat. In the original version, score 0 is described as ‘Alert; keenly responsive’. The expert panel decided that the Norwegian term adekvat was the most suitable as it covered both våken and adekvat.
In the non-validated Norwegian NIHSS version, the Norwegian term våken is used for score 0. Here, the term adekvat was used for score 1, which is a lower level of consciousness. In the pilot test, several informants reported that the guide in the validated version of the NIHSS was clearer on the scoring of consciousness.
The original version uses the term ‘non-paretic hand’ when testing responses to commands. The forward translators used various translations in Norwegian, such as ikke-paretisk hånd, ikke-paretiske hånden, neve på ikke-affisert side and hånden uten parese.
We placed a large emphasis on harmonisation with the non-validated version.
The forward translation sent to the qualified translator included the Norwegian term den friske hånden. This term is known from the non-validated Norwegian version and was therefore chosen as a validated translation. We placed a large emphasis on harmonisation with the non-validated version.
The patient’s horizontal eye movements are scored in the NIHSS. The original version uses the term ‘best gaze’. The forward translators suggested various Norwegian translations (blikk, blikkbevegelser, øyebevegelser and blikkøvelser). The term blikk refers more to the direction the patient is looking, and the expert group therefore considered it most correct to use blikkbevegelse as a validated translation.
In the original version, several terms, such as ‘oculocephalic’ and ‘caloric testing’, are used to test reflexive movements of the eyes. These are known concepts in neurology, but require specialist knowledge or training to be able to understand what they mean.
In the original version, the term ‘visual field’ is used when scoring the patient’s vision. All four forward translators used the Norwegian term synsfelt, which is a well-known medical term and was therefore chosen for the validated translation.
In the original version, the score for ‘motor arm’ and ‘motor leg’ is recorded as untestable (UN) in the case of amputation. In the non-validated Norwegian version, the corresponding condition is scored with the value 0. In order to remain true to the English original version, we included the Norwegian term for ‘untestable’ in the validated version. The change did not have any consequences for the overall NIHSS score.
Language adapted to Norwegian culture
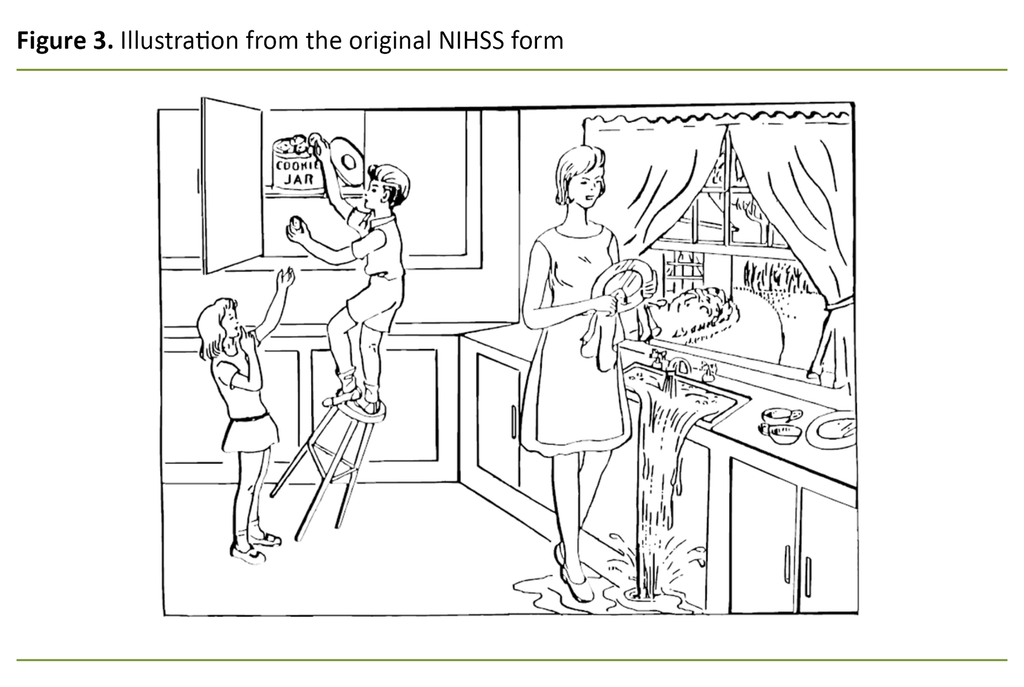
In the original English version of the NIHSS, the patient’s language and motor speech are tested using standardised illustrations and text sheets. For language comprehension, pictures of a glove, key, cactus, chair, feather and hammock are used, as well as a scene from a kitchen in a home.
The expert panel agreed to keep all the English illustrations as they are recognisable in Norwegian culture.
The expert panel agreed to keep all the English illustrations as they are recognisable in Norwegian culture. The picture of a glove could be interpreted as a hand, and this was accepted as a correct answer in the original version (7). Figures 2 and 3 show the illustrations from the original English version of the NIHSS, all of which were retained in the validated Norwegian version.
With regard to the text sheets, we changed two of the terms to make them a better fit with Norwegian culture. One term was ‘baseball player’, which was changed to the Norwegian term for a basketball player, as Norwegians are more familiar with basketball than baseball.
The second term, ‘huckleberry’, was changed to the Norwegian word for gooseberry for two reasons. One reason is that the huckleberry is not found in Norway, but gooseberries are. The second reason is that the Norwegian word for gooseberry (stikkelsbær) contains two s-sounds, which is helpful when testing for dysarthria. Table 2 shows the text words in both the English and the validated translated version, adapted to Norwegian culture.
In the pilot test, the test subjects tested out the illustrations and text sheets in the validated version and were positive about using them. Two test subjects commented that the text sheets could not be used, but it turned out that the patients who were tested scored 2 on language function. This indicates severe aphasia, where speech is difficult or impossible. It was therefore not possible to test the use of the text words in these patients.
‘Extinction’ is the term used in the original version where the patient’s attention is assessed. The forward translators suggested four different terms in Norwegian: extinction og uoppmerksomhet, neglekt, redusert oppmerksomhet/neglekt and ekstinksjon og uoppmerksomhet.
In the non-validated Norwegian version, the terms ‘neglect/extinction’ are used. The expert panel chose redusert oppmerksomhet/neglekt in the forward translation. Neglekt is a term used in neurology, and one that medical personnel are familiar with.
On some of the sub-scale exams in the NIHSS, the original version provides an opportunity to describe the reason for ‘untestable’, while the non-validated Norwegian version uses score = 0 instead. The expert panel’s experience from practice shows that clinicians prefer to describe the reason for untestability in the form. The expert panel therefore decided to follow the original version.
In the original version, the title ‘the investigator’ is used for the person administering the NIHSS. The person administering the NIHSS was given at the top of the form. In the first Norwegian validated version, which was sent to the translator, the Norwegian term testleder was chosen for ‘the investigator’.
The translator back translated this to ‘testing leader’. The expert panel was not satisfied with this term and considered the Norwegian term for clinician (kliniker) instead. After harmonisation with the non-validated Norwegian version, the group decided not to give a title.
Through contact with the stroke units that were asked to pilot test the validated version, nurses and doctors were concerned that the validated version might take longer to administer than the non-validated one, and that the overall score might change. The pilot test showed that these concerns were unfounded.
Discussion
In the translation work, the project group chose an expert panel who mostly had extensive experience in administering the NIHSS. This expertise helped to ensure satisfactory validity of content where the language was culturally adapted to practice (15, 16). One weakness of the translation process was that it was not possible to contact the original authors. Using the original author is an important part of validation work (10, 11, 13, 17).
This expertise helped to ensure satisfactory validity of content where the language was culturally adapted to practice.
There is no standard method for translation validation and cultural adaptation, but the existing methods are largely in agreement (10, 13). Several researchers discuss the importance of regularly revising validation and cultural adaptation, as language and culture change over time (11, 18, 19).
Practitioners and researchers were together on the validation
The expert panel placed an emphasis on harmonising the validated version with the non-validated one, since it had already been translated into Norwegian and used in practice for a number of years. As such, the hope was that it could be perceived as valid and thereby support the validated version.
In pilot testing, face validity is tested, where healthcare professionals provide concrete feedback on terms and wording that may be difficult to understand (14). The face validity reveals whether formulations and terms are understandable to the target group (14).
In this way, a pilot test will ensure that a validated translation is adapted to the culture in which it is to be used (20). A pilot test can be carried out as a focus group interview with several clinicians together. Researchers stress that inaccuracies are easier to detect through conversation (16).
In our project group, conducting a focus group interview was considered to be resource-intensive because it would involve interviews with nurses and doctors from several stroke units in Norway.
Six of the nine stroke units invited to participate in the pilot test agreed to take part. Those that did not participate said that their unit was too busy, and that the testing could not be prioritised. Nevertheless, the result provided an impression of what worked well and what should be changed.
We respected both the original version and the existing translated version
Throughout the project work, attention was focused on bias as a result of the existing translated version having been used in Norway for a number of years. It was therefore particularly important to compare the non-validated and the validated versions in the pilot test.
The pilot test revealed that two test subjects had different scores for the patient’s outcome. It would have been easier to have a conversation about the reason for the different scoring, which could have led to suggestions for more comprehensible formulations. Other studies support the use of such a method (18, 19).
Elements of our version differ from the non-validated version
Most countries that have validated the NIHSS in their own language and culture have included the same illustrations and text sheets as the original version. Some countries have adapted them to their own culture (9, 21, 22).
In our project, the expert panel decided to retain the same illustrations and text sheets with a few adaptations. This means that the validated Norwegian version of the NIHSS is significantly different from the non-validated one, which does not use illustrations or text sheets. The pilot test showed that the scale did not take longer to administer when illustrations and text sheets were used.
The pilot test showed that the scale did not take longer to administer when illustrations and text sheets were used.
Nevertheless, this change in practice is difficult to implement without guidance in a transitional phase. Another significant difference between the validated and non-validated versions is the scoring of ‘untestable’. In the non-validated version, ‘untestable’ is given a score of 0, while the validated version describes ‘untestable’ using the descriptor ‘IT’ (which stands for untestable in Norwegian) as the score. None of the test subjects in the pilot test commented on this difference in scoring.
The project group’s starting point was a desire to develop standardised training in the use of the NIHSS. The Norwegian validated version is the basis for an e-learning course that Norwegian health trusts can now use. The e-learning course will facilitate quality assurance in the use of the NIHSS in practice.
Conclusion
Validation of the NIHSS was required to ensure culturally appropriate language. In the validation process, it was important to involve stroke units in pilot testing the form and guide and to use an expert panel with experienced doctors and nurses.
The result is a Norwegian validated version of the NIHSS form and guide that is true to the original English version, and also harmonised with the non-validated Norwegian version.
We would like to thank former stroke nurse Morten Iversen at Kongsberg Hospital, Vestre Viken Hospital Trust for his important contribution to the validation work.
References
1. Helsedirektoratet. Nasjonal faglig retningslinje for behandling og rehabilitering ved hjerneslag. Oslo: Helsedirektoratet; 2017. Available at: https://helsedirektoratet.no/retningslinjer/hjerneslag (downloaded 27.03.2020).
2. National Institute of Neurological Disorders and Stroke. Know stroke, know the signs, act in time. USA: Department of Health & Human Services; 2019. Available at: http://www.strokecenter.org/wp-content/uploads/2011/07/NIH_Stroke_Scale_Booklet.pdf (downloaded 27.03.2020).
3. Criddle LM, Bonnono C, Fisher SK. Standardizing stroke assessment using the National Institutes of Health Stroke Scale. Journal of Emergency Nursing. 2003;29(6):541–6.
4. Bruno A, Saha C, Williams LS. Percent change on the National Institutes of Health Stroke Scale: a useful acute stroke outcome measure. Journal of Stroke and Cerebrovascular Diseases. 2009;18(1):56–9.
5. Fassbender K, Balucani C, Walter S, Levine SR, Haass JG. Streamlining of prehospital stroke management: the golden hour. Lancet Neurol. 2013;12:585–96.
6. Hage V. The NIH stroke scale: a window into neurological status. Nursing Spectrum. 2011;24:44–9.
7. Martin-Schield S, Siegler JE, Kumar AD, Lyden P. Troubleshooting the NIHSS: question-and-answer session with one of the designers. International Journal of Stroke. 2015;10(8):1284–6.
8. Domínguez RV, Vila JF, Augustovski JF, Irazola V, Castillo PA, Escalante RR, et al. Spanish cross-cultural adaptation and validation of the National Institutes of Health Stroke Scale. Mayo Clinic Proceedings. 2006;81(4):476–80.
9. Cicero C, Pontes-Neto OM, Neville LS, Mendes HF, Minenes DF, Mariano DC, et al. Validation of the National Institutes of Health Stroke Scale, Modified Rankin Scale and Barthel Index in Brazil: the role of cultural adaptation and structured interviewing. Cerebrovasc Dis. 2009;27(2):119–22.
10. World Helath Organization (WHO). Process of translation and adaptation of instruments. WHO; 2016. Available at: https://www.who.int/substance_abuse/research_tools/translation/en/ (downloaded 27.03.2020).
11. Herdman M, Fox-Rushby J, Badia X. A model of equivalence in the cultural adaptation of epidemiological measurement instruments. Revista de Saúde Pública. 2007; 41(4). Available at: https://kopernio.com/viewer?doi=10.1590%2FS0034-89102006005000035&token=WzE2MTU2ODQsIjEwLjE1OTAvUzAwMzQtODkxMDIwMDYwMDUwMDAwMzUiXQ.WDA_1N2h1kkym0y_mBax-IFZqqE (downloaded 27.03.2020).
12. Wang WL, Lee HL, Fetzer SJ. Challenges and strategies of instrument translation. Western Journal of Nursing Research. 2006;28(3):310–21.
13. Ljoså TM, Jacobsen HB, Granan LP, Reme, SE. ReKS modifiserte oversettelsesmetode for spørreskjema. Frem-og-tilbake oversettelse med kulturell tilpasning og lingvistisk validering. Oslo: Regional Kompetansetjeneste for smerte (ReKS), Avdeling for smertebehandling, Oslo universitetssykehus (OUS); 2013. Available at: https://oslo-universitetssykehus.no/seksjon/Regional-kompetansetjeneste-for-smerte/Documents/ReKS%20modifiserte%20oversettelsesprosedyre%20for%20sp%C3%B8rreskjema%2018sept2015.pdf (downloaded 27.03.2020).
14. Polit DF, Beck CT. Nursing research: generating and assessing evidence for nursing practice. 10. utg. Philadelphia, PA: Wolters Kluwer; 2017.
15. Newell R, Burnard P. Research for evidence-based practice in healthcare. Chichester: Wiley-Blackwell; 2011.
16. Gjersing L, Caplehorn JRM, Clausen T. Cross-cultural adaptation of research instruments: language, setting, time and statistical considerations. BMC Biomedical Research Methodology. 2010;10:13. Available at: https://kopernio.com/viewer?doi=10.1186%2F1471-2288-10- 13&token=WzE2MTU2ODQsIjEwLjExODYvMTQ3MS0yMjg4LTEwLTEzIl0.IO- CP12dmPhIzd-3SmzOO5ADVC8 (downloaded 27.03.2020).
17. Beaton DE, Bombardier C, Guillermin F, Ferraz MB. Guidelines for the process of cross-cultural adaptation of self-report measures. Spine. 2000;25(24):3186–91.
18. Reichenheim ME, Moraes CL. Operationalizing the cross-cultural adaptation of epidemiological measurement instruments. Revista de Saúde Pública. 2007;41(4):665–73. Available at: https://kopernio.com/viewer?doi=10.1590%2FS0034-89102006005000035&token=WzE2MTU2ODQsIjEwLjE1OTAvUzAwMzQtODkxMDIwMDYwMDUwMDAwMzUiXQ.WDA_1N2h1kkym0y_mBax-IFZqqE (downloaded 27.03.2020).
19. Utne I, Grov EK, Kjerland LE, Rønning M, Rodrigues-Aranda C, Rasmussen HL, et al. Oversettelse og kulturell tilpasning av Attentional Function Index (AFI). Sykepleien Forskning. 2017;12(64646):(e-64646). DOI: 10.4220/Sykepleienf.2017.64646
20. Nord R, Jerpseth H, Fagermoen MS. Betydning av pilotundersøkelse før validering av oversatte instrumenter. Nordisk Sygeplejeforskning. 2012;1(2):45–55. Available at: https://www.idunn.no/nsf/2012/01/art06 (downloaded 27.03.2020).
21. Dancer S, Brown AJ, Yanase LR. National Institutes of Health Stroke Scale in plain English is reliable for novice nurse users with minimal training. J Emerg Nurs. 2017;43(3):221–7. Available at: https://ezproxy2.usn.no:2169/science/article/pii/S0099176716302124 (downloaded 27.03.2020).
22. Berger K, Weltermann B, Kolominsky-Rabas P, Meves S, Heuschmann P, Böhner J, et al. Untersuchung zur Reliabilität von Schlaganfallskalaen. Fortschr. Neurol. Psychiat. 1999;67(2):81–6.

























Comments