Medication reviews on admission of residents to nursing homes
A large proportion of the residents at nursing homes did not receive a medication review when they were admitted, despite this being a statutory requirement.
Background: According to the regulations relating to medication management for facilities and health personnel providing healthcare (Forskrift om legemiddelhåndtering for virksomheter og helsepersonell som yter helsehjelp), a systematic medication review is to be carried out upon admission of new long-term nursing home residents. The regulations do not specify what time frame ‘upon admission’ covers.
Objective: The objective of this study was to examine how much time it took from the point of admission until the first medication review was carried out at the nursing homes featured in the study.
Method: We carried out a retrospective observational study at three nursing homes in Vestland county. Residents in long-term care at the selected nursing homes as of 1 January 2017 (the date when the regulations entered into effect) or later, were considered suitable for inclusion in the study. Information such as age, gender, date when the resident was allocated a place and the date of the first medication review after the allocation of a long-term nursing home place was retrieved from the residents’ electronic health records.
Results: A total of 77 people with a median age of 87 (71–104) were included in the study. There was considerable variation between the three nursing homes but, in total, 49 per cent of the residents had received a medication review within the first month after admission. The time it took from admission until the first medication review varied from one to twenty months. Seventeen per cent of the residents had not received a medication review at the time of collecting the data for the study, and the median period of residency for these people was nine (2–25) months.
Conclusion: For approximately half of the residents in the study, it took more than one month after admission to the nursing home until a medication review was carried out. The results suggest that there is a need to improve routines for carrying out medication reviews when residents are allocated a long-term nursing home place.
The term ‘drug-related problem’ is defined as ‘an event involving drug therapy that actually or potentially interferes with desired health outcomes’ (Pharmaceutical Care Network Europe, cited in 1). Drug-related problems include prescription of unsuitable drugs, unnecessary drug use, adverse effects or drug interactions (1).
Elderly patients who take many medications have a higher risk of being affected by drug-related problems. A Norwegian study of drug use in 41 Norwegian nursing homes found an average of 2.6 drug-related problems per resident (2). Adverse effects were twice as frequent among elderly patients in comparison to younger patients, and they were also more serious among the elderly (3, 4).
It is estimated that approximately 10 per cent of hospital admissions of elderly patients are the result of adverse drug reactions (5–7). A Norwegian study indicates that adverse drug reactions are the cause of death in one in five elderly hospital patients (8).
Systematic medication review is a method used to quality assure individual patients’ medication use by identifying drug-related problems, optimising the efficacy of medication and thereby reducing adverse drug events (1).
Systematic medication reviews have been shown to contribute to the identification and resolution of drug-related problems; however, substantially differing results have been found in studies that examine the effect of medication reviews on patient outcomes such as quality of life and mortality (2, 9, 10).
In Report to the Storting (white paper) No. 18 (2004–2005), it was proposed that a pilot project focusing on medication review be carried out to ensure effective and correct drug treatment (11). This measure was followed up in the National Health and Care Services Plan and in the White Paper on Medicinal Products — Correct use –better health, in which it was recommended that medication reviews should be performed systematically in nursing homes (12, 13).
Furthermore, correct use of medications in nursing homes is one of the priorities in the National Patient Safety Programme 2014–2018. In the programme, it is recommended that cross-disciplinary, structured medication reviews are carried out upon admission of new residents and thereafter on a regular six-monthly basis. The programme also provides background information and tools for carrying out medication reviews (14).
The recommendation on medication reviews resulted in the following amendment to the regulations relating to medication management for facilities and health personnel providing healthcare (Forskrift om legemiddelhåndtering for virksomheter og helsepersonell som yter helsehjelp), which entered into effect on 1 January 2017:
‘The healthcare facility is to ensure that a systematic medication review is carried out for long-term nursing home residents upon admission and thereafter at least once a year. Beyond this, a medication review is to be carried out when deemed necessary in order to ensure proper treatment.’ (authors’ italics) (15). According to the regulations, medication reviews must be performed by a doctor, either alone or in collaboration with other health personnel (15).
The Norwegian Directorate of Health has published a guide for medication reviews Veileder om legemiddelgjennomganger, which contains suggestions for medication review processes (16). In practice, there is a relatively large variation in how medication reviews are performed, particularly in relation to which occupational groups are involved, the degree of cooperation between occupational groups and the degree of patient involvement (17, 18).
When carrying out medication reviews in cross-disciplinary teams, the health occupational groups involved will fill different roles. It will often be the responsibility of the registered nurse (RN) or primary care provider to assess the patient’s level of function, communicate with the patient’s family and follow up changes set out in the medication review. The pharmacist provides special expertise in drugs and their adverse effects, while the doctor has responsibility for writing prescriptions and decision-making in the medication review process.
According to a report from the Norwegian Directorate of Health based on data from the IPLOS Register (individual-based nursing and healthcare statistics), 58 per cent of long-term nursing home residents aged 67 or over received a medication review in 2019 (19).
However, it is not known what percentage of Norwegian nursing home residents receive a medication review upon admission. It is important to carry out a medication review upon admission because medication errors often occur during transitions of care (20).
The objective of the study
The objective of this study was to examine how much time it takes from the point of admission to a nursing home until the first medication review is carried out. This type of examination can provide knowledge that is useful in efforts to improve the quality of services.
Method
Design and participants
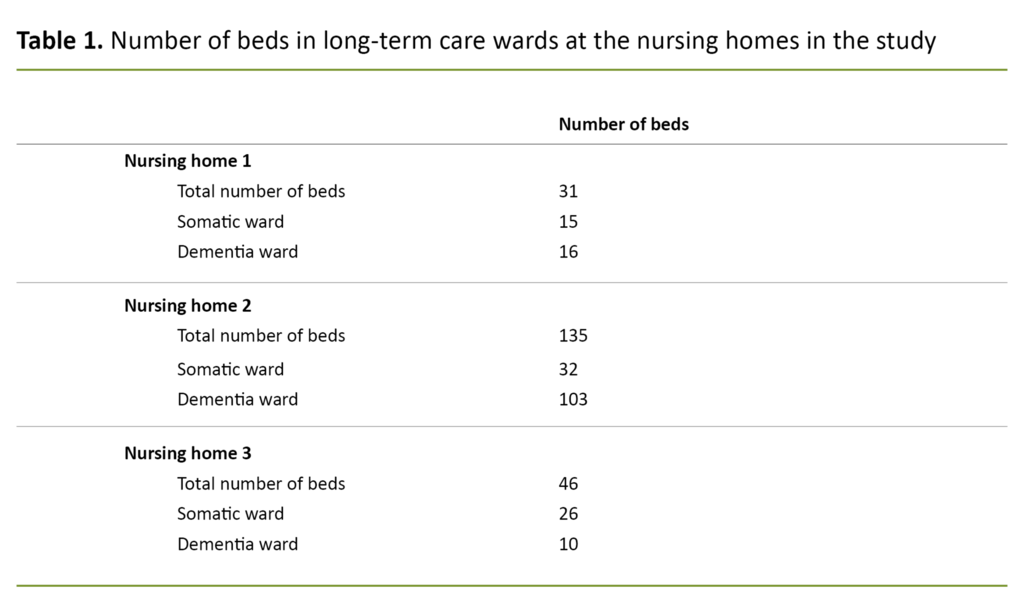
We carried out a retrospective observational study (21) of three randomly selected nursing homes of varying sizes in Vestland county (Table 1). At each of the nursing homes, we included residents who fulfilled the following criteria: 1) they were residents at the nursing home in question at the time we collected the data, and 2) they had been allocated a place in long-term care on or after 1 January 2017.
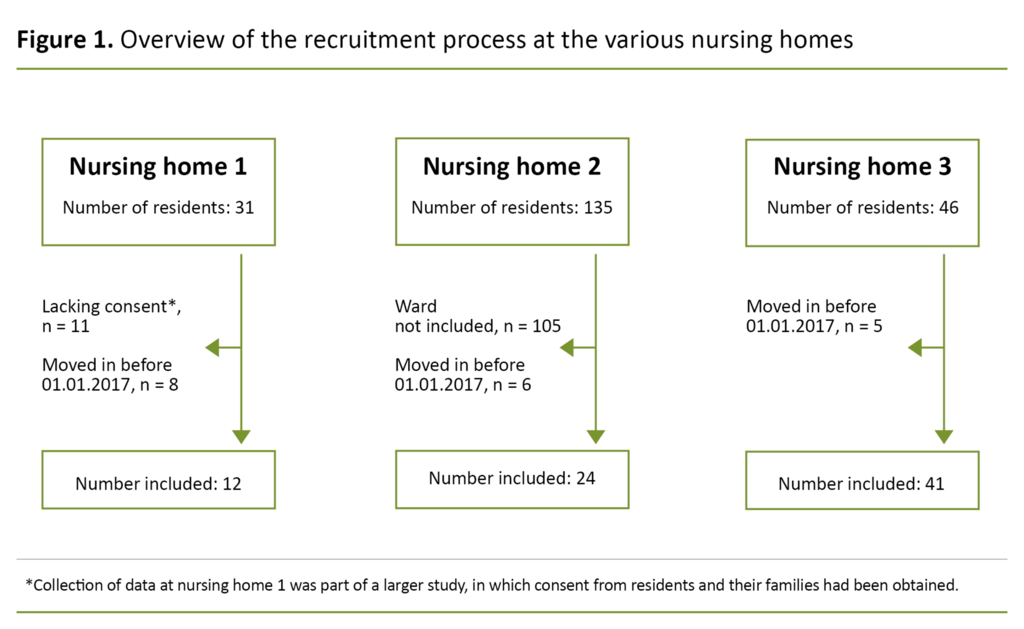
The sample at nursing home 1 included residents who were already participating in a larger study on medication reviews at the nursing home, which 20 of the nursing home’s 31 residents and, in some cases, their family members, had consented to participate in. Of these residents, 12 had been admitted after 1 January 2017 and were therefore included in this sub-study.
At nursing home 2, we included residents in two randomly selected wards in the study. Out of a total of 30 residents in these two wards, 24 had been allocated a place in long-term care on or after 1 January 2017 and were therefore included in this study. At nursing home 3, all of the residents who fulfilled the criteria were included (n = 41). Figure 1 shows an overview of the sample.
Collection of data
We collected data in the period between December 2018 and March 2019 for nursing home 1 and in September 2019 for nursing homes 2 and 3. All of the data were retrieved from the residents’ electronic health records at the nursing homes. We recorded the details on a standard form to ensure that the same type of information was collected at all of the participating nursing homes.
The following details were retrieved: information about the resident’s age, gender, date of allocation of a long-term nursing home place (month), type of ward (dementia or somatic ward), and the date that the first medication review was carried out after the resident was allocated a place.
If the electronic health records revealed that the medication review had been carried out within three months prior to the resident being allocated a long-term place, this was also recorded. At nursing home 1, we also collected information about which occupational groups had participated in the medication review.
Data analysis
The study population was described using descriptive statistics with median values, maximum and minimum values for continuous variables (age), and quantity and frequency (%) for categorical variables (gender).
The primary outcome measure was the percentage of residents who had received medication reviews upon admission, where ‘upon admission’ was defined as meaning in the course of the first month after the resident moved in to the nursing home.
The secondary outcome measure was the percentage of residents who had received medication reviews in the period from admission up until the time data was collected, the median time from admission until the first medication review was carried out and the median duration of residency for residents who had not received a medication review.
The categorical outcome measure is described as the frequency (quantity and percentage), while the continuous outcome measure is described by the median value, the maximum and the minimum value.
If the medication review had been carried out during a short-term stay at the same nursing home during the three months prior to being allocated a long-term place, we registered the medication review ‘upon admission’ as carried out. This applied to three of the residents. When we calculated the median time between admission and the first medication review for these residents, the medication review was registered as being carried out during the first month of the resident’s stay. We used IBM SPSS version 27 for the statistical analysis.
Ethics and personal privacy protection
A master’s student collected the data at nursing home 1, while the data at nursing homes 2 and 3 were collected by undergraduate nursing students who were in clinical placement at the nursing homes in question. At nursing home 1, we obtained the consent of residents or their families, as they were participating in a larger research project in which directly identifiable personal data had been collected.
At the other two nursing homes, we did not register directly or indirectly identifiable personal data and therefore it was not necessary to obtain the participants’ consent. The Norwegian Centre for Research Data considered the project to be in accordance with personal privacy legislation (reference number 61134), and the Regional Committees for Medical and Health Research Ethics concluded that the project was not subject to a submission requirement (reference number 2018/1141).
Results
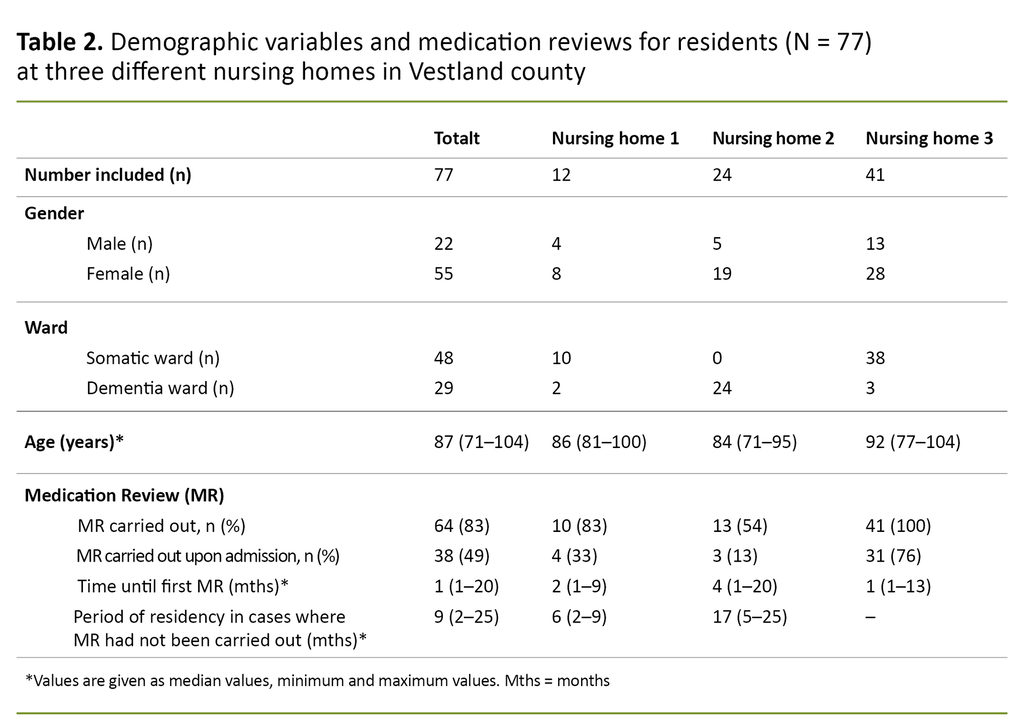
A total of 77 residents were included in the study (Table 2). The median age of the participants was 87 (71–104), and 71 per cent were women (n = 55). A total of 38 per cent (n = 29) of the participants were patients in dementia wards (Table 2).
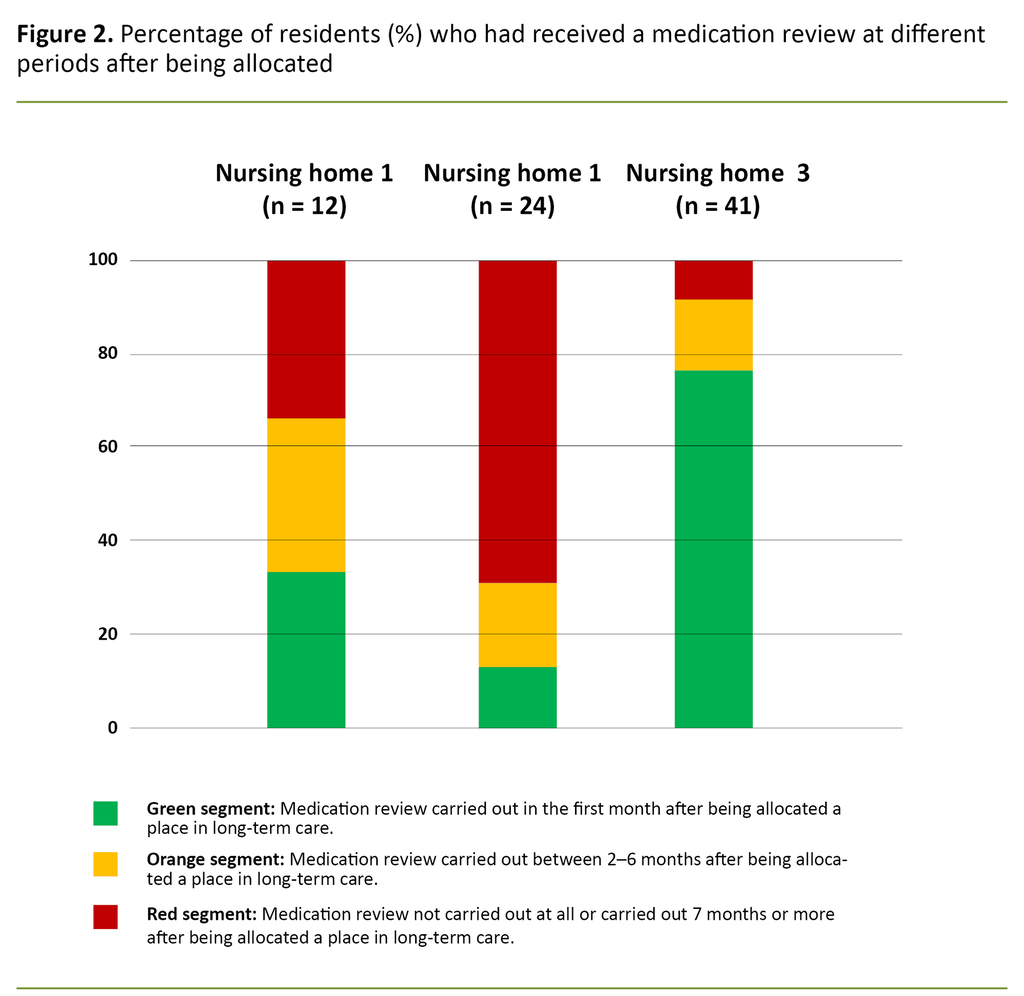
The percentage of the residents who had received a medication review in the course of the first month after admission varied from 13 to 76 per cent at the various nursing homes (Figure 2, Table 2). The percentage of the residents who had received a medication review during their entire period of residency was 83 per cent, and this varied between 54 and 100 per cent at the different nursing homes (Table 2).
The percentage of the residents who had received a medication review during their entire period of residency was 83 per cent.
For the residents who had received a medication review, the time between admission and the first medication review varied from one to thirteen months. At the time the data were collected, a total of 17 per cent (n = 13) of the residents had not received a medication review after being allocated a place in long-term care. These were residents at nursing home 1 (n = 2, both informants were patients in the somatic ward) or nursing home 2 (n = 11), and the median period of residency for these residents was nine (2–25) months (Table 2).
At nursing home 3, all of the residents included in the study had received medication reviews (Table 2). At this nursing home, the medication review had been carried out more than a month after admission for ten of the residents (24 per cent), and in this group the median time until the first medication review was carried out was seven (2–13) months. All of the ten residents who had not received a medication review during the first month after admission had moved in at a time that coincided with Easter or summer holidays, i.e. March–April or May–August. Those who had been admitted at other times of the year had all received a medication review during the same month that they moved in.
At nursing home 1, a doctor and an RN participated in all of the medication reviews. Pharmacists had not participated in any of the medication reviews, and neither had input been obtained from pharmacists prior to carrying out the medication reviews. At nursing homes 2 and 3, no data were collected on who took part in medication reviews.
Discussion
At the three nursing homes we examined in this study, only 49 per cent of the residents had received a medication review during the first month after admission. The percentage of residents that had received a medication review in conjunction with admission varied considerably between the various nursing homes. There were also significant variations in the time it took before a medication review was carried out, both between the various nursing homes and for different residents at the same nursing home.
Vague guidelines
The regulations relating to medication management for facilities and health personnel providing healthcare specify that medication reviews are to be carried out ‘upon admission’, but there is no further explanation of what the term ‘upon admission’ covers and available guidelines are also vague on this point. The Norwegian Directorate of Health’s report on correct use of medications for elderly patients, residents of nursing homes and patients in home-based nursing care states that medication reviews should be carried out within two weeks of admission (22).
In the National Patient Safety Programme’s package of measures aimed at correct use of medications in nursing homes, the proposal for procedures states that a medication review should be carried out within four weeks after a resident moves in to a nursing home (14).
In order to carry out a satisfactory medication review, personnel must have sufficient time to become acquainted with the individual resident, so that a thorough assessment can be carried out prior to the medication review. Consequently, it is to be expected that it will take some time from the point of admission until a medication review can be carried out.
The time it takes for personnel to become properly acquainted with residents can vary. It can be particularly time-consuming to build up a solid basis for carrying out a satisfactory medication review when dealing with residents who have impaired cognitive function and whose ability to express themselves is reduced as a consequence, both in relation to adverse effects and the efficacy of drug treatment. The guide for medication reviews (Veileder om legemiddelgjennomganger) does not distinguish between different types of wards in their recommendation for time limits for carrying out medication reviews (16).
Our study was not designed to examine whether there are differences in practice between different types of wards, and therefore it is not possible to determine whether our observations reflect actual differences between different types of wards or variations between nursing homes.
The results showed that nursing home 2 carried out the lowest percentage of medication reviews in the first month after residents had been allocated a long-term place. All of the residents included were patients in a dementia ward.
However, it was also at this nursing home that we found the highest percentage of residents that had not received a medication review (54 per cent), which can indicate a lack of routines for carrying out medication reviews rather than a conscious choice to wait until the personnel were better acquainted with the residents.
Significant differences between nursing homes
In total, only about half of the residents received a systematic medication review in the first month after admission, but there were significant differences between the nursing homes. The time it took until the first medication review was carried out was seven months or more for 31 per cent of the residents.
There were significant differences between the nursing homes.
Seventeen per cent of the residents had not received a medication review at all after moving to the nursing home. Of these, six had been living at the healthcare facility for over a year, and should therefore have received an annual medication review in accordance with the requirements in the regulations (15).
We do not have any information about why medication reviews were not carried out in individual cases. Possible causes may be a lack of routines for medication reviews at the healthcare facility in question, or that it was not considered necessary for the individual resident, for example, because they were not taking many medications.
Neither do we have any information about the reasons for the observed differences between the nursing homes, but different routines at the various nursing homes and a lack of continuity and access to medical services may be possible causes (23).
Earlier studies have shown that an appropriate division of roles, knowledge about responsibility, communication, cooperation between occupational groups and low turnover of personnel are key factors for achieving good quality in healthcare services (23, 24).
It is the healthcare facility manager’s responsibility to ensure that systematic medication reviews are carried out according to the regulations, which includes the responsibility to ensure that there are good routines in place (15). The National Patient Safety Programme’s guide for medication reviews at nursing homes points out that it is the role of the individual RN to identify residents who require medication reviews (14).
The fact that it is the responsibility of the individual RN to identify which residents require medication reviews does not, however, replace the systematic work of carrying out medication reviews that should be incorporated into the healthcare facility’s routines.
This may indicate difficulties in maintaining routines in conjunction with holiday periods.
At one of the nursing homes, it was exclusively the residents who had been admitted at Easter or during the summer holidays who had not received a medication review in conjunction with admission.This may indicate difficulties in maintaining routines during holiday periods.
The failure to carry out medication reviews on admission cannot be explained by the possibility that a resident had already received a medication review while staying in short-term care at the nursing home and awaiting a long-term place. Only three of the residents had received medication reviews while staying in short-term care at the nursing home in the three months prior to being allocated a long-term place.
On the whole, the findings from this study show that a large percentage of residents in Norwegian nursing homes do not receive medication reviews on admission, despite this being a statutory requirement (15).
There is a need to improve routines for carrying out systematic medication reviews at Norwegian nursing homes.
Systematic medication reviews on admission are a tool for reducing medication errors and inappropriate use of medications in individual patients and, therefore, the lack of a medication review poses a threat to patient safety (20). Our findings suggest that there is a need to improve routines for carrying out systematic medication reviews at Norwegian nursing homes.
Strengths and limitations
One significant weakness in this study is the lack of information concerning the individual residents’ medication use at nursing homes 2 and 3. We cannot rule out the possibility that the lack of medication reviews at these nursing homes is due to the fact that the residents did not use medications, but we regard this as relatively unlikely based on earlier studies that describe the medication use of residents in Norwegian nursing homes (2, 25–27).
The study is also limited by the fact that we have only collected data from three nursing homes and that the recruitment strategy was somewhat different for each nursing home. Nevertheless, we consider the findings to be transferable, because the nursing homes are located in three different municipalities and the percentage of residents who had received annual medication reviews corresponded with the national average for 2019, i.e. 58 per cent or more (19).
The fact that the three nursing homes in the study roughly correspond with the national average for annual medication reviews gives us reason to believe that our findings for medication reviews on admission are also typical of the average Norwegian nursing home.
The data that have been collected for this study can only be used to assess how much time it took from admission until the medication review was carried out, not to identify the causes for any lack of medication reviews. Identifying possible factors that are associated with the carrying out of medication reviews would be of major interest in further studies.
Conclusion
The results of this study show that for roughly half the residents, it took more than one month after admission before the medication review was carried out. In other words, only half of the residents received a medication review upon admission in accordance with the regulations.
The findings in this study suggest that there is a need to improve routines for carrying out medication reviews when residents are allocated long-term nursing home places.
We would like to thank the students for their help collecting the data, and also the clinical nurse educators and management at the nursing homes.
References
1. Ruths S, Viktil KK, Blix HS. Klassifisering av legemiddelrelaterte problemer. Tidsskr Nor Laegeforen. 2007;127(23):3073–6.
2. Fog AF, Kvalvaag G, Engedal K, Straand J. Drug-related problems and changes in drug utilization after medication reviews in nursing homes in Oslo, Norway. Scandinavian Journal of Primary Health Care. 2017;35(4):329–35.
3. Cresswell KM, Fernando B, McKinstry B, Sheikh A. Adverse drug events in the elderly. Br Med Bull. 2007;83:259–74.
4. Mallet L, Spinewine A, Huang A. The challenge of managing drug interactions in elderly people. Lancet. 2007;370(9582):185–91.
5. Gosney M, Tallis R. Prescription of contraindicated and interacting drugs in elderly patients admitted to hospital. Lancet. 1984;2(8402):564–7.
6. Grymonpre RE, Mitenko PA, Sitar DS, Aoki FY, Montgomery PR. Drug-associated hospital admissions in older medical patients. Journal of the American Geriatrics Society. 1988;36(12):1092–8.
7. Beard K. Adverse reactions as a cause of hospital admission in the aged. Drugs Aging. 1992;2(4):356–67.
8. Ebbesen J, Buajordet I, Erikssen J, Brors O, Hilberg T, Svaar H, et al. Drug-related deaths in a department of internal medicine. Archives of Internal Medicine. 2001;161(19):2317–23.
9. Alldred DP, Kennedy MC, Hughes C, Chen TF, Miller P. Interventions to optimise prescribing for older people in care homes. The Cochrane Database of Systematic Reviews. 2016;2.
10. Lehnbom EC, Stewart MJ, Manias E, Westbrook JI. Impact of medication reconciliation and review on clinical outcomes. Ann Pharmacother. 2014;48(10):1298–312.
11. Meld. St. 18 (2004–2005). Rett kurs mot riktigere legemiddelbruk. Oslo: Helse- og omsorgsdepartementet; 2005.
12. Meld. St. 16 (2010–2011). Nasjonal helse- og omsorgsplan (2011–2015). Oslo: Helse- og omsorgsdepartementet; 2011.
13. Meld. St. 28 (2014–2015). Legemiddelmeldingen – Riktig bruk – bedre helse. Oslo: Helse- og omsorgsdepartementet; 2015.
14. Pasientsikkerhetsprogrammet 2014–2018. «I trygge hender 24/7». Available at: http://www.pasientsikkerhetsprogrammet.no/ (downloaded 25.01.2021).
15. Forskrift 3. april 2008 nr. 320 om legemiddelhåndtering for virksomheter og helsepersonell som yter helsehjelp. Available at: https://lovdata.no/dokument/SF/forskrift/2008-04-03-320?q=legemiddelgjennomgang (downloaded 25.01.2021).
16. Helsedirektoratet. Veileder om legemiddelgjennomganger. Oslo: Helsedirektoratet; 2015. Available at: https://www.helsedirektoratet.no/veiledere/legemiddelgjennomganger/Legemiddelgjennomganger%20%E2%80%93%20Veileder.pdf/_/attachment/inline/dabc9103-bba9-4a92-9382-12e6f9160e2d:5850d4e841293ea9caeab645a9dfe0f3a3d5ca74/Legemiddelgjennomganger%20%E2%80%93%20Veileder.pdf (downloaded 26.02.2021).
17. Bell HT, Granas AG, Enmarker I, Omli R, Steinsbekk A. Nurses' and pharmacists' learning experiences from participating in interprofessional medication reviews for elderly in primary health care – a qualitative study. BMC Fam Pract. 2017;18(1):30.
18. Bulajeva A, Labberton L, Leikola S, Pohjanoksa-Mantyla M, Geurts MM, de Gier JJ, et al. Medication review practices in European countries. Res Social Adm Pharm. 2014;10(5):731–40.
19. Helsedirektoratet. Legemiddelgjennomgang hos beboere på sykehjem i 2019. Oslo: Helsedirektoratet; 2020. Available at: https://www.helsedirektoratet.no/statistikk/kvalitetsindikatorer/kommunale-helse-og-omsorgstjenester/legemiddelgjennomgang-hos-beboere-p%C3%A5-sykehjem (downloaded 26.02.2021).
20. Olsen RM, Devik SA. Legemiddelbruk og pasientsikkerhet. En oppsummering av kunnskap. 2016. Available at: https://omsorgsforskning.brage.unit.no/omsorgsforskning-xmlui/handle/11250/2415062 (downloaded 26.02.2021).
21. Polit D, Beck CT. Nursing Research: generating and assessing evidence for nursing practice. 11th ed. Philadelphia: Wolters Kluwer Health; 2019.
22. Helsedirektoratet. Riktig legemiddelbruk til eldre pasienter/beboere på sykehjem og i hjemmetjenesten. Oslo: Helsedirektoratet; 2011. IS-1887. Available at: https://helsedirektoratet.no/Lists/Publikasjoner/Attachments/255/Riktig-legemiddelbruk-til-eldre-pasienter-beboere-pa-sykehjem-og-i-hjemmesykepleien-IS-1887.pdf (downloaded 26.02.2021).
23. Melby L, Ågotnes G, Ambugo EA, Førland O. Kartlegging av medisinskfaglig tilbud i sykehjem og heldøgns omsorgsboliger. Senter for omsorgsforsknings rapportserie nr. 3/2019. Available at: https://ntnuopen.ntnu.no/ntnu-xmlui/bitstream/handle/11250/2596428/Rapport%2003_19_web-Final.pdf?sequence=1&isAllowed=y (downloaded 26.02.2021).
24. Førland O, Rostad HM. Variasjon og uønsket variasjon i kvalitet i omsorgstjenestene. En kunnskapsoppsummering. Senter for omsorgsforsknings rapportserie nr. 4/2019. Available at: https://ntnuopen.ntnu.no/ntnu-xmlui/bitstream/handle/11250/2624074/rapport_04_2019v1_final2.pdf?sequence=1&isAllowed=y (downloaded 26.02.2021).
25. Halvorsen KH, Selbaek G, Ruths S. Trends in potentially inappropriate medication prescribing to nursing home patients: comparison of three cross-sectional studies. Pharmacoepidemiology and Drug Safety. 2017;26(2):192–200.
26. Kersten H, Ruths S, Wyller TB. Farmakoterapi i sykehjem. Tidsskr Nor Laegeforen. 2009;129(17):1732–5.
27. Kirkevold O, Engedal K. Is covert medication in Norwegian nursing homes still a problem? A cross-sectional study. Drugs Aging. 2009;26(4):333–44.




















Comments